Understanding the Growing Concern Around Microplastics
Microplastics have become an unavoidable part of modern life.
They contaminate food, drinking water, air, and everyday consumer products.
Scientific research now confirms that these microscopic plastic particles can enter the human body and accumulate in tissues.
This discovery has raised legitimate concerns about their impact on hormone-sensitive organs, including the prostate.
Men increasingly search for clear, evidence-based information on how environmental exposures influence prostate health.
This article explains how microplastics affect prostate health and function, using current scientific knowledge without exaggeration or fear-based messaging.
You will learn how microplastics enter the body, what researchers know about their interaction with prostate tissue, and why inflammation and hormonal disruption matter.
The goal is education, not alarm.
Why Microplastics and Prostate Health Are Linked
Environmental health research has shifted dramatically in the last decade.
Scientists no longer focus solely on diet and genetics when studying prostate disorders.
Instead, they examine cumulative exposure to synthetic chemicals and particles.
Microplastics represent one of the most widespread and least understood exposures.
Studies now confirm that microplastics can cross biological barriers.
They have been detected in blood, lungs, digestive tissue, and reproductive organs.
The prostate is especially vulnerable because it depends on precise hormonal regulation.
Even minor disruptions in androgen signaling, inflammation, or oxidative balance can influence prostate function over time.
Research also shows that plastics often carry endocrine-disrupting chemicals such as bisphenols and phthalates.
These compounds can mimic or interfere with natural hormones.
Understanding how microplastics affect prostate health and function helps men make informed lifestyle and environmental choices.
It also supports prevention-focused discussions grounded in science rather than speculation.
This article synthesizes current evidence, explains biological mechanisms, and clearly distinguishes established findings from ongoing research questions.
How Microplastics Enter the Body and Reach Internal Organs
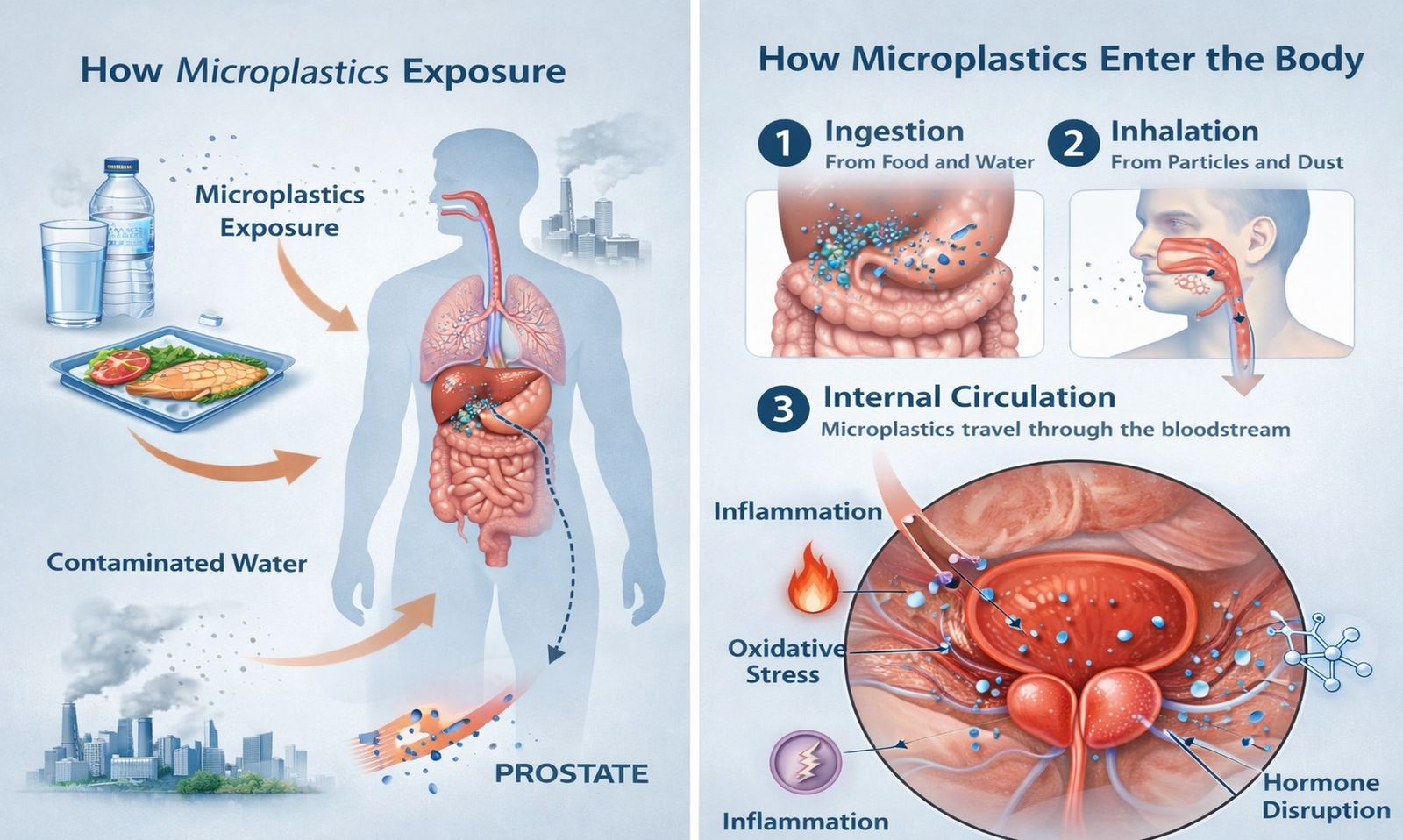
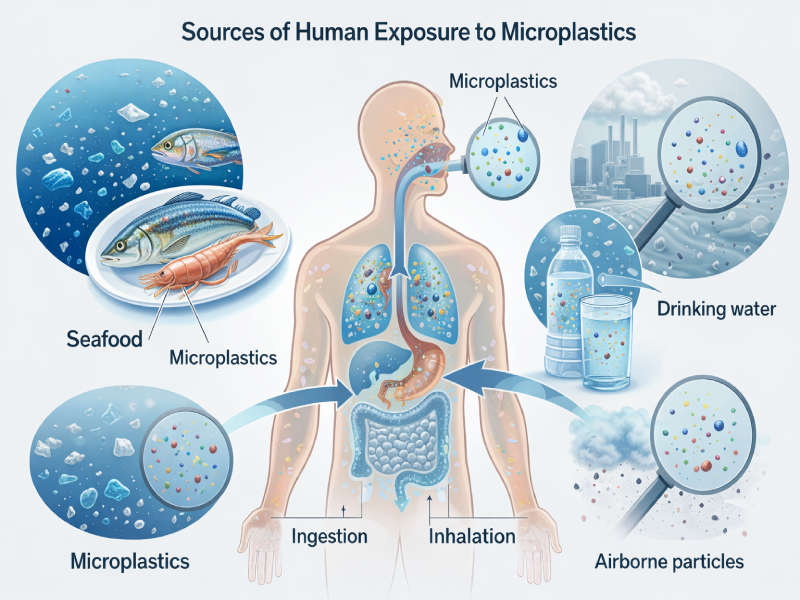
Microplastics enter the body primarily through ingestion and inhalation.
Drinking water, seafood, packaged foods, and airborne dust represent major exposure sources.
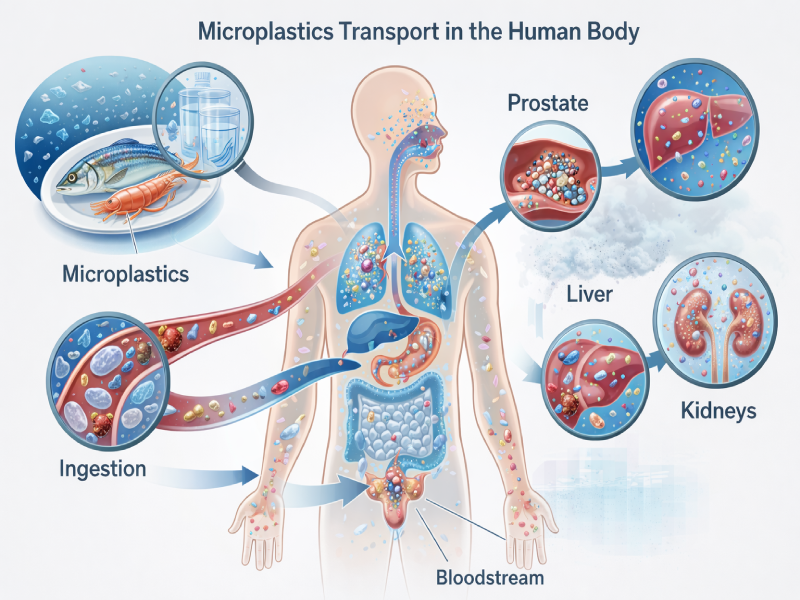
Once inside the body, smaller particles may cross intestinal or pulmonary barriers.
Animal and laboratory studies show that particles under 10 micrometers can migrate through tissues.
Microplastics rarely act alone.
They often transport chemical additives, heavy metals, and persistent organic pollutants.
These combined exposures increase biological relevance.
The prostate, as a hormonally regulated organ, may respond to these stressors through inflammation and cellular signaling changes.
How microplastics affect prostate health and function refers to their potential to accumulate in prostate tissue, promote inflammation, disrupt hormone signaling, and contribute to oxidative stress. While direct clinical causation remains under investigation, experimental studies support biological mechanisms linking microplastic exposure to prostate dysfunction.
Understanding environmental exposure requires reliable, science-based guidance.
Independent educational resources on endocrine disruptors and environmental toxicology can help contextualize emerging research and reduce misinformation.
Biological Mechanisms Linking Microplastics to Prostate Health
The prostate relies on androgen signaling to regulate growth and secretory function.
Disruptions to this system can alter normal cellular behavior.
Plastic-associated chemicals often act as endocrine disruptors.
They may bind to hormone receptors or interfere with testosterone metabolism.
Microplastics also promote chronic low-grade inflammation.
Inflammatory signaling plays a recognized role in benign prostatic hyperplasia and other prostate conditions.
Oxidative stress represents another concern.
Laboratory studies demonstrate increased reactive oxygen species in cells exposed to microplastic particles.
While human clinical data remains limited, these mechanisms provide biological plausibility.
Researchers emphasize caution, not conclusions.
Evidence From Human and Experimental Studies
Human data on microplastics and prostate health is still developing.
However, tissue analysis studies confirm direct exposure.
Experimental research offers mechanistic insight.
Cell culture studies show inflammatory and oxidative responses in prostate cells exposed to plastic particles.
Animal models suggest endocrine disruption may influence prostate structure and gene expression.
These findings guide hypotheses for future epidemiological research.
Importantly, no study claims microplastics alone cause prostate disease.
Researchers consistently frame findings as contributory and context-dependent.
This distinction supports responsible health communication.
Lifestyle and Environmental Risk Context
Microplastics represent one element of cumulative exposure.
Diet, physical activity, chemical contact, and metabolic health interact continuously.
Reducing exposure does not require extreme measures.
Practical steps include minimizing plastic food packaging, improving ventilation, and supporting antioxidant-rich diets.
Public health research increasingly emphasizes exposure reduction rather than elimination.
This balanced approach aligns with current evidence.
Conclusion: How Microplastics Affect Prostate Health and Function
Understanding how microplastics affect prostate health and function requires nuance.
Current science does not support panic or deterministic conclusions.
What evidence does show is biological plausibility.
Microplastics can reach prostate tissue, carry endocrine-disrupting chemicals, and promote inflammatory responses.
The prostate’s dependence on hormonal balance makes it sensitive to environmental stressors.
Chronic low-level exposure may influence long-term prostate function, especially when combined with other risk factors.
Research continues to evolve.
Large-scale human studies are still needed to clarify exposure thresholds and clinical relevance.
In the meantime, informed awareness empowers better decision-making.
Men who understand environmental health risks can adopt realistic exposure-reduction strategies without fear or misinformation.
Scientific literacy, not alarm, remains the most effective protective tool.
For men seeking structured nutritional and lifestyle support focused on prostate health, targeted educational solutions may help complement healthy habits.

Scientific References Summary Table
| Authors (Year) | Full Title | Source | Key Findings |
|---|---|---|---|
| Leslie et al. (2022) | Discovery and quantification of plastic particles in human blood | Environment International | Confirms systemic microplastic exposure |
| Ragusa et al. (2021) | Plastic particles in human tissues | Environmental Research | Identifies microplastics in internal organs |
| Rochester (2013) | Bisphenol A and human health | Reproductive Toxicology | Endocrine disruption mechanisms |
| McDougall et al. (2019) | Environmental exposures and inflammation | PNAS | Links chronic exposure to inflammatory pathways |
Medical Disclaimer
This article is for informational purposes only.
I am not a medical doctor, and this content does not replace professional medical advice, diagnosis, or treatment.
Always consult a qualified healthcare provider regarding prostate health or medical concerns.