Your Phone May Be Making You Gain Weight While You Sleep
You eat well. You exercise. You go to bed at a decent hour. And yet, the scale refuses to budge — or worse, it keeps creeping upward. Sound familiar?
Millions of people share this frustrating experience, and the answer may not lie in your diet or workout routine at all. A growing body of peer-reviewed research now points to an unexpected culprit hidden in plain sight: the artificial blue light emitted by your smartphone, tablet, laptop, and television screen — especially during the hours before bed.
Scientists at Harvard Medical School, the American Journal of Medicine, and JAMA Internal Medicine have published compelling evidence linking nighttime light exposure to significant disruptions in the hormones that regulate fat storage, appetite, and metabolism. This is not a fringe theory. It is supported by thousands of clinical data points.
In this article, you will discover exactly how blue light from screens causes weight gain at night, the precise biological mechanisms at work, what poor sleep quality does to your hunger hormones, and the practical steps you can take to begin reversing this cycle — starting tonight.
Whether you have 10 pounds or 50 pounds to lose, understanding this connection may be the single most important shift in perspective you make all year.

To understand why your nightly screen habits may be sabotaging your body composition, we first need to understand what happens inside your body the moment that blue light hits your eyes — and why your brain interprets it as a signal to stop burning fat.
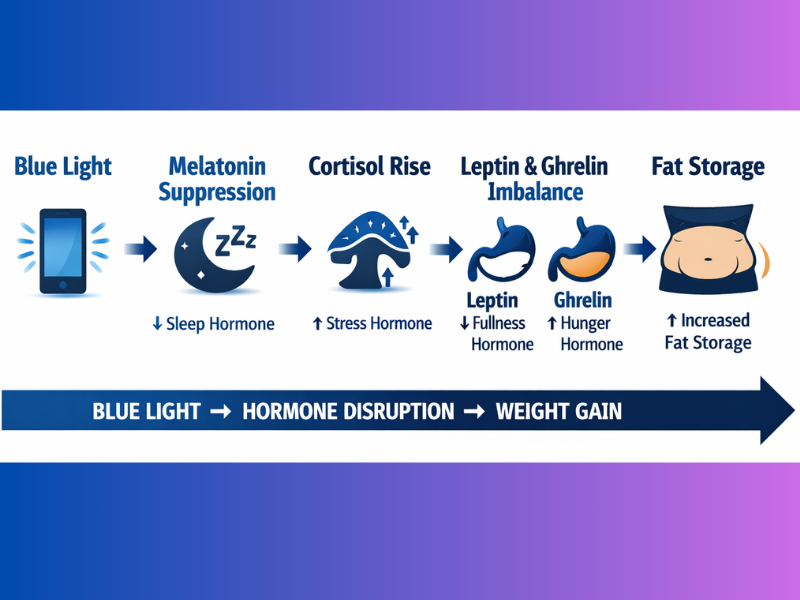
Blue light from screens causes weight gain at night by suppressing melatonin production and disrupting the body’s circadian rhythm. This disruption elevates cortisol, impairs insulin sensitivity, and dysregulates the hunger hormones leptin and ghrelin — increasing appetite, slowing overnight metabolism, and promoting fat storage. Exposure to blue light before or during sleep significantly increases obesity risk, particularly abdominal fat accumulation.
Want to break the cycle of sleep-disrupted weight gain? Discover a natural, science-backed formula designed to support deep, restorative sleep and healthy overnight fat metabolism
The Science Behind Blue Light, Hormones, and Fat Storage
Your body operates on a precise internal clock known as the circadian rhythm. This 24-hour biological cycle governs everything from when you feel tired to when your body releases fat-burning hormones during the night. Blue light — the high-energy visible light spectrum emitted by LED screens — directly interferes with this clock.
When your eyes detect blue light, they send a signal to the suprachiasmatic nucleus (SCN), the brain’s master clock, telling it that it is still daytime. Your brain responds by suppressing melatonin — the hormone that normally signals your body to enter recovery and fat-burning mode at night.
A landmark 2019 study published in JAMA Internal Medicine (Park et al.) found that women who slept with artificial light at night — including from a television or phone — had a significantly higher risk of developing obesity compared to those who slept in darkness. The researchers tracked over 43,000 women and observed increases in body mass index, waist circumference, and total body fat mass.
At the same time, light-driven cortisol disruption tells the body to store energy as fat rather than burn it. Insulin sensitivity drops, so glucose that would normally enter your muscle cells for energy gets redirected into fat cells instead — particularly around the abdomen.
The compounding effect is devastating for anyone trying to lose weight: you are hungrier the next day, less able to process carbohydrates, and your body is physiologically primed to hold onto every calorie as stored fat.
Key Ways Nighttime Screen Exposure Promotes Weight Gain
Why Deep NREM Sleep Is Your Body’s Most Powerful Fat-Burning Window
Most people focus exclusively on diet and exercise when they try to lose weight. But scientists increasingly recognize that the hours between 11 PM and 3 AM — during which the body should be cycling through deep, slow-wave NREM (Non-Rapid Eye Movement) sleep — represent the most metabolically active period of the 24-hour cycle.
A 2022 review published in Nutrients (Papatriantafyllou et al.) confirmed that sleep deprivation — whether from quantity or quality — directly impairs fat loss and makes it harder to maintain weight loss over time. The researchers found that disrupted sleep altered adipose tissue distribution, increased inflammatory markers, and dysregulated multiple fat-metabolism pathways.
During deep NREM sleep, the pituitary gland releases the largest pulse of growth hormone the body produces in a 24-hour period. This pulse is essential for lipolysis — the process of breaking down stored fat and releasing it into the bloodstream as fuel. When blue light delays or fragments your entry into deep NREM sleep, this hormone pulse is blunted or skipped entirely.
The result is not simply feeling tired the next morning. It is a measurable reduction in your body’s ability to burn fat overnight, regardless of how well you ate that day.
The Hunger Hormone Effect: Why Poor Sleep Makes You Overeat the Next Day
A pivotal study from the American Journal of Medicine (Thorogood et al., 2011) and follow-up research published in BMJ Open Sport & Exercise Medicine (Coughlin et al., 2018) established a clear link between sleep deprivation and dysregulation of the two hormones that govern appetite: leptin and ghrelin.
Leptin tells your brain when you have eaten enough and signals your body to release stored fat for energy. Ghrelin does the opposite — it drives hunger and promotes fat storage. After a night of disrupted, light-polluted sleep, leptin levels fall while ghrelin levels surge.
In practical terms, this means you wake up significantly hungrier than you would after a night of restorative sleep. You are drawn to calorie-dense foods, your willpower over food choices is reduced, and your body simultaneously holds onto its fat reserves more aggressively. This is why people who consistently sleep poorly tend to gain weight progressively — even when their diet has not changed.
The blue light connection closes this loop: by preventing your body from producing adequate melatonin and entering restorative sleep stages, screens at night set off a cascade that makes you hungrier, slower, and fatter — one bad night at a time.
How Much Blue Light Does It Take to Disrupt Your Sleep and Metabolism?
You do not need to stare at a screen for hours to experience meaningful hormonal disruption. Research shows that as little as 30 to 60 minutes of screen exposure in the two to three hours before bed can measurably suppress melatonin and delay the onset of slow-wave sleep.
The problem is compounded by modern habits: the average adult spends over seven hours per day in front of screens, with a significant portion of that time occurring in the evening. Smartphones, streaming services, and social media are engineered to maximize engagement precisely during the hours when your brain should be winding down.
Televisions and computers emit lower levels of blue light per unit area than smartphones held close to the face — but all contribute meaningfully to circadian disruption when used in the hours before sleep. Even low-level ambient lighting with a significant blue spectrum has been shown to delay melatonin onset.
Evidence-Based Strategies to Reduce Blue Light’s Impact on Your Weight
Natural Compounds That Support Deep Sleep and Overnight Fat Metabolism
Beyond behavioral changes, certain natural plant-derived compounds have demonstrated evidence-based benefits for sleep quality, melatonin production, and metabolic function during sleep. Understanding these ingredients helps you make informed decisions about supporting your body’s nightly repair processes.
Valerian root has been studied specifically for its effect on sleep quality in adults. A randomized, placebo-controlled clinical trial published in Menopause (Taavoni et al., 2011) found that valerian significantly improved sleep quality in postmenopausal women, a population particularly vulnerable to sleep disruption and associated metabolic changes.
Humulus lupulus (hops) has demonstrated sedative properties in peer-reviewed research. Franco et al. (2012) published findings in Acta Physiologica Hungarica confirming the sedative efficacy of hops extract, particularly in combination with valerian.
5-HTP (Griffonia simplicifolia) is a clinically-validated serotonin precursor. A review published in Alternative Medicine Review (Birdsall, 1998) confirmed 5-HTP as a clinically effective way to raise serotonin levels, supporting mood stability and sleep onset — both of which are disrupted by blue light exposure.
Berberine has been studied for its effects on metabolic function, including insulin sensitivity and blood pressure. A 2021 systematic review in Complementary Therapies in Clinical Practice (Santos-Parker et al.) highlighted berberine’s role in supporting healthy metabolic markers — directly relevant to the insulin disruption caused by poor sleep.
Inulin supports gut microbiome health and has been shown to influence appetite-regulating hormones. A comprehensive review published in Food & Function (Yu et al., 2023) detailed inulin’s multiple health benefits, including its prebiotic effects on metabolic regulation.
Lutein functions as a blue-light filter at the cellular level. Research published in Archives of Biochemistry and Biophysics (Junghans et al., 2001) showed that macular pigments including lutein act as natural filters against high-energy blue light — supporting the body’s ability to limit blue light’s disruptive impact on the retina’s circadian signaling pathway.
The Bottom Line: Your Screen Habit May Be the Hidden Reason You Can’t Lose Weight
The evidence is now difficult to ignore. Blue light from screens does not simply make it harder to fall asleep — it actively reprograms your body’s hormonal environment in ways that promote fat storage, increase appetite, impair glucose metabolism, and reduce your capacity to burn fat during the night.
This understanding reframes the entire weight loss conversation. For decades, the advice was simple: eat less, move more. And while caloric balance and physical activity remain important, they are not the complete picture. If your hormonal signals — cortisol, insulin, leptin, ghrelin, growth hormone, and melatonin — are chronically disrupted by poor sleep quality driven by light pollution, your body is working against your efforts, not with them.
The good news is that this cycle is reversible. By reducing evening screen exposure, optimizing your sleeping environment for complete darkness, and supporting your body with evidence-based natural compounds that promote deep, restorative sleep, you can begin to recalibrate the hormonal environment that governs your weight.
Small, consistent changes in your nighttime routine can lead to meaningful improvements in sleep quality — and, by extension, in how your body manages fat overnight. You do not need to be perfect. You simply need to start reducing the interference between your evening habits and your body’s natural fat-burning window.
Your results will depend on your individual circumstances, overall health, and consistency with both behavioral and nutritional support. But the science is clear: protecting your sleep is one of the most powerful steps you can take toward reaching and maintaining a healthy body weight.
If disrupted sleep has been holding back your weight loss progress, explore a natural formula developed to support deep, restorative sleep and healthy overnight metabolism.

Scientific References Summary
| # | Authors / Year | Journal | Key Finding | Relevance |
|---|---|---|---|---|
| 1 | Park et al. (2019) | JAMA Internal Medicine | Artificial light at night during sleep associated with significantly higher obesity risk in women — increased BMI, waist circumference, and body fat. | Direct link: nighttime light → obesity |
| 2 | Coughlin et al. (2018) | BMJ Open Sport & Exercise Medicine | Sleep deprivation directly associated with increased obesity risk in adults through hormonal and metabolic disruption. | Confirms sleep-weight gain connection |
| 3 | Papatriantafyllou et al. (2022) | Nutrients | Sleep deprivation impairs fat loss and weight maintenance; disrupted sleep alters fat distribution and metabolic pathways. | Validates NREM sleep as fat-burning window |
| 4 | Buxton & Marcelli (2011) | Current Opinion in Clinical Nutrition & Metabolic Care | Sleep and obesity are directly linked; insufficient sleep is a significant contributor to excess body fat accumulation. | Establishes sleep–obesity causation |
| 5 | Taavoni et al. (2011) | Menopause | Valerian root significantly improved sleep quality in postmenopausal women in a randomized placebo-controlled trial. | Supports valerian for sleep quality |
| 6 | Franco et al. (2012) | Acta Physiologica Hungarica | Hops (Humulus lupulus) demonstrated measurable sedative effects in human subjects. | Supports hops for sleep onset |
| 7 | Birdsall (1998) | Alternative Medicine Review | 5-HTP is a clinically effective serotonin precursor with demonstrated benefits for sleep and mood regulation. | Supports 5-HTP for sleep chemistry |
| 8 | Santos-Parker et al. (2021) | Complementary Therapies in Clinical Practice | Systematic review confirms berberine’s role in supporting insulin sensitivity and healthy metabolic markers. | Supports berberine for metabolic function |
| 9 | Lobo et al. (2022) | Metabolites | Spirulina consumption associated with improved glycemic responses in healthy adults. | Supports metabolic regulation |
| 10 | Junghans et al. (2001) | Archives of Biochemistry & Biophysics | Lutein and zeaxanthin act as blue-light filters in biological membranes, limiting high-energy visible light damage. | Supports lutein for blue light protection |
| 11 | Yu et al. (2023) | Food & Function | Inulin demonstrates multiple health benefits including prebiotic activity and metabolic regulation via gut microbiome. | Supports inulin for appetite regulation |
| 12 | Thorogood et al. (2011) | American Journal of Medicine | Systematic review confirming that aerobic exercise and sleep quality together, not in isolation, produce the most significant metabolic improvements. | Context for multi-factor weight loss |
Medical Disclaimer
The information provided in this article is for educational and informational purposes only. I am not a medical doctor, licensed nutritionist, or registered dietitian. The content of this article does not constitute medical advice, diagnosis, or treatment, and should not be used as a substitute for professional medical advice from a qualified healthcare provider.
Always consult your physician or a qualified health professional before making changes to your diet, sleep routine, supplement regimen, or lifestyle, particularly if you are pregnant, nursing, taking prescription medication, or managing a diagnosed medical condition.
Affiliate Disclosure: This article may contain affiliate links. If you click on a link and make a purchase, I may receive a commission at no additional cost to you. All recommendations are based on research and editorial judgment, and I only promote products I believe may offer genuine value.
The scientific references cited in this article are from peer-reviewed publications and are included for informational context. Individual results vary. Supplements are not intended to diagnose, treat, cure, or prevent any disease.